Atypical antipsychotics vs typical antipsychotics
by egpat 06 Aug 2019
Chlorpromazine as well as clozapine, both used for treatment of schizophrenia. Is there any difference in their usage and preference? Of course, there is a difference. Clozapine is preferred over chlorpromazine many of the times. Former drug is an atypical antipsychotic while later is a typical antipsychotic.
Apart from this little difference, these two categories of drugs have many variations in their chemical nature, receptor profile and possible side effects. So let’s discuss all these in detail here.
Types of generation
First point of difference between these drugs is about their generation. Within the classification of antipsychotics , drugs can be listed into two categories such as first generation and second generation antipsychotics. Typical antipsychotics are old generation drugs that are developed before 1970. That’s why these drugs are considered as first generation antipsychotics.

Contrarily, atypical antipsychotics are new generation drugs that are developed after 1970. These medications are generally called as second generation antipsychotics. Even this terminology such as first generation and second generation is not preferred it’s better to regard them as typical and atypical antipsychotics.
Whether clozapine is atypical antipsychotic?
Yes, even this drug is invented in the year of 1959 it got FDA approval in late 1989 almost after 30 years. Due to its multiple receptor selectivity and less extrapyramidal side effects, it is classified as atypical antipsychotic.
Receptor selectivity
This is again a significant point of difference between these categories of drugs. Typical antipsychotics like chlorpromazine and haloperidol mainly act on dopamine receptors as antagonists particularly at D2 receptors. With some similarity, atypical antipsychotics also bind to the dopamine receptors as antagonists. But their selectivity is broader among the dopamine receptors such that they bind not only to D2 receptors but also to D1 and D4 receptors located in CNS.
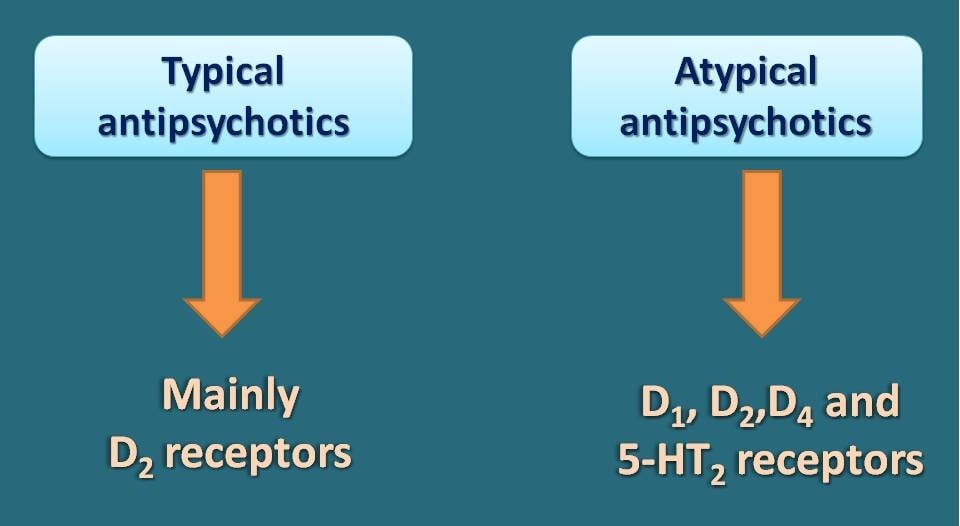
Interestingly, these atypical antipsychotics bind to other receptors such as muscarinic acetylcholine receptors , 5-HT2 receptors.
Action of atypical antipsychoics on multiple receptors may add an advantage in their clinical efficacy as they have less prone to induce extrapyramidal side effects.
Chemical nature
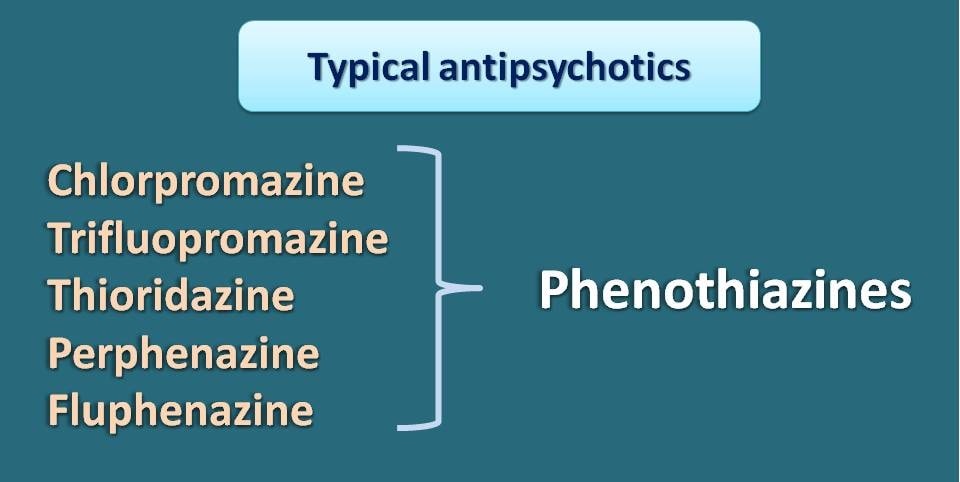
Typical antipsychotics can be grouped into few of the chemical categories and they really show structural features related to their dopamine receptor selectivity and action. For example, drugs like chrlopromazine, trifluopromazine, thioridazine and fluphenazine all belong to a chemical class called phenothiazines .
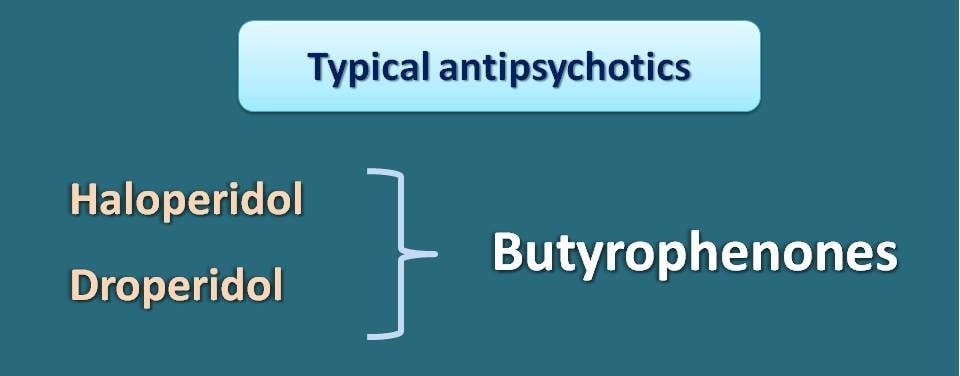
Similarly haloperidol and droperidol belong to chemical class of butyrophenones.
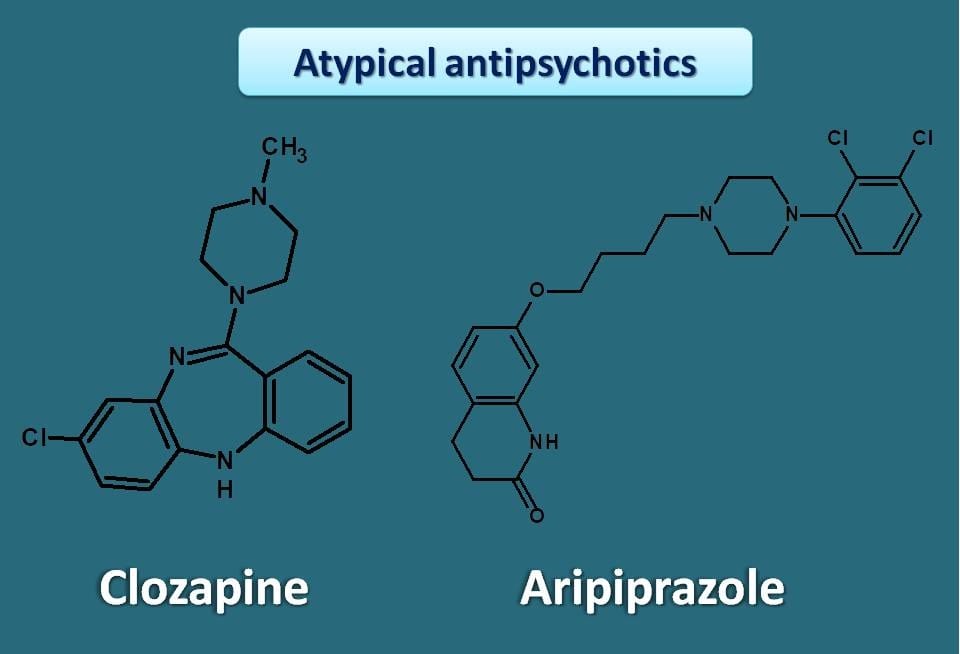
Quite oppositely, atypical antipsychotics belong to diverse chemical group each drug having less structural relevance. For example, clozapine contains dibenzazepine ring while aripiprazole has a different structure with quinoline ring.
Side effects
This is really a point to consider where atypical antipsychotics raise their flagship in providing less extrapyramidal side effects over typical antipsychotics.

But this doesn’t mean that atypical antipsychotics are completely free from serious side effects and in fact, few of the drugs in this category have shown significant side effects like weight gain and diabetes. They may also increase cholesterol levels in the body on prolonged use.
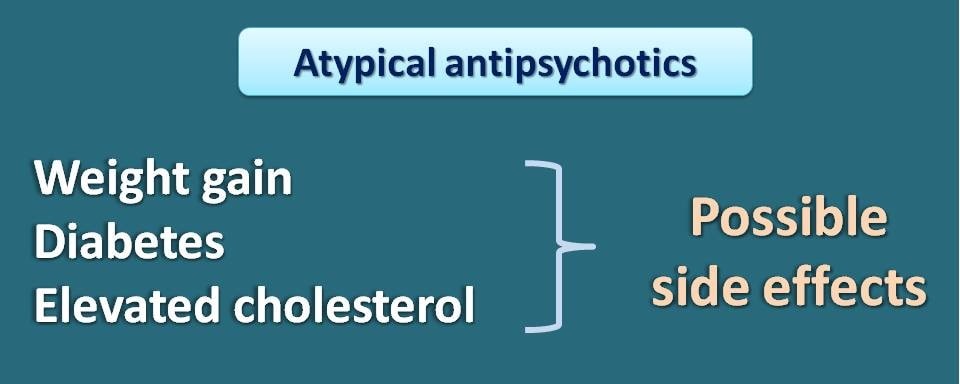
With few exceptions, it has been shown that many of the atypical antipsychotics are safer and don’t produce more serious motor side effects as typical antipsychotics do.
Therapeutic efficacy
Typical antipsychotics are useful in treating positive symptoms of schizophrenia like hallucinations and delusions. Unfortunately they are less effective against negative symptoms of schizophrenia such as social withdrawal and reduced emotional responses in the patient.
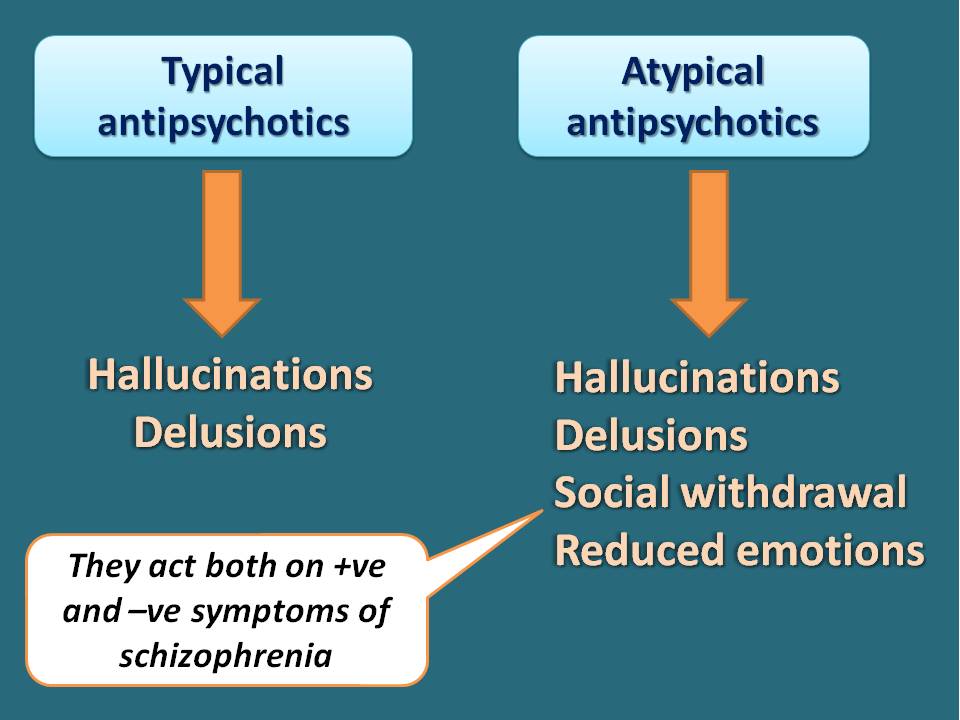
In this context, atypical antipsychotics again played a key role in ameliorating these negative symptoms in the patients which are generally treatment resistant to the typical antipsychotics. Here is a video on the 5 difference between typical and atypical antipsychotics.
So that’s all about few of the important differences between typical and atypical antipsychotics.